Some of the NIPT tests look for missing snippets of chromosomes. For every 15 times they correctly find a problem, they are wrong 85 times.
After a year of fertility treatments, Yael Geller was thrilled when she found out she was pregnant in November 2020. Following a normal ultrasound, she was confident enough to tell her 3-year-old son his “brother or sister” was in her belly.
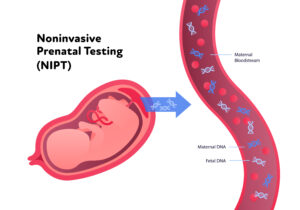
Noninvasive parental testing NIPT concept. Vector flat healthcare illustration. Genetic test. Baby in womb, blood vessel, dna spiral symbol. Design for healthcare, pharmacy, family planning
But a few weeks later, as she was driving her son home from school, her doctor’s office called. A prenatal blood test (NIPT) indicated her fetus might be missing part of a chromosome, which could lead to serious ailments and mental illness.
Sitting on the couch that evening with her husband, she cried as she explained they might be facing a decision on terminating the pregnancy. He sat quietly with the news. “How is this happening to me?” Ms. Geller, 32, recalled thinking.
The next day, doctors used a long, painful needle to retrieve a small piece of her placenta. It was tested and showed the initial result was wrong. She now has a 6-month-old, Emmanuel, who shows no signs of the condition he screened positive for.
Ms. Geller had been misled by a wondrous promise that Silicon Valley has made to expectant mothers: that a few vials of their blood, drawn in the first trimester, can allow companies to detect serious developmental problems in the DNA of the fetus with remarkable accuracy.
In just over a decade, the tests have gone from laboratory experiments to an industry that serves more than a third of the pregnant women in America, luring major companies like Labcorp and Quest Diagnostics into the business, alongside many start-ups.
The tests initially looked for Down syndrome and worked very well. But as manufacturers tried to outsell each other, they began offering additional screenings for increasingly rare conditions.
The grave predictions made by those newer tests are usually wrong, an examination by The New York Times has found.
January 2, 2022, www.nytimes.com, Sarah Kliff and
Click here to read the entire article.