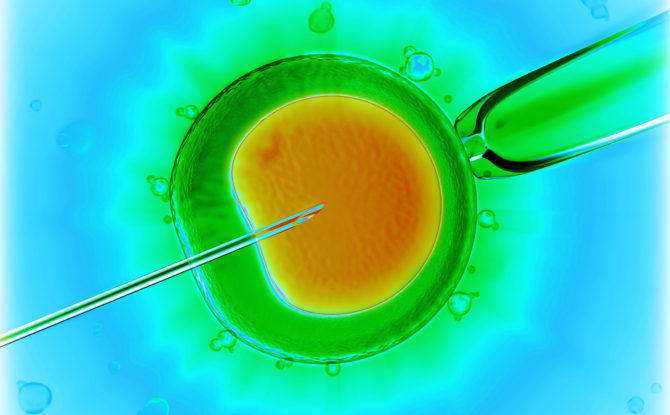
IVF Add Ons – This is no way to treat patients desperate for a baby.
There are few things as unsettling as sitting in an in vitro fertilization clinic hearing you need a team of experts — embryologists, lab techs and nurses along with a reproductive endocrinologist — to help you become pregnant.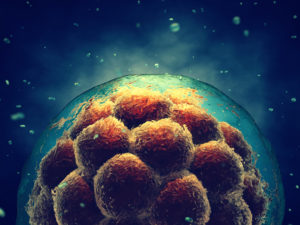
What comes next can be a blur. First, you meet with the clinic’s financial counselor to assess whether you have enough money for a complex, invasive $15,000-$20,000 IVF cycle. What follows are drug injections, blood tests, invasive ultrasounds, surgical egg retrieval, and fertilization ahead of an embryo transfer. Before your first hormone shot, you’re well into head-spinning, unfamiliar territory.
Then the doctor tells you there are “add-ons” you might want to consider.
Might you have interest in endometrial scratching? What about vasodilation, human growth hormones, intralipids, assisted hatching, oocyte activation, physiological intracytoplasmic sperm injection, or embryo glue? Post-fertilization, there is also embryo pre-implantation genetic testing to consider. Interested?
These extras come with price tags ranging from hundreds to thousands of dollars. All are presented as ways to increase your chances of a pregnancy. What are you willing to try? What can you afford? The ball is in your court.
This is no way to treat patients at their most vulnerable.
That’s the conclusion my colleagues and I arrive at in a new paper on the ethics and regulation of IVF add-ons.
An add-on is anything that is not essential to carry out an IVF cycle. Such measures, patients are told, will improve the likelihood of a live birth — and yet our examination revealed a startling absence of robust research into the effectiveness and the safety of these add-ons. Despite this, their use is widespread, and regulation of them is minimal.
The most expensive add-on category is pre-implantation genetic testing. These tests were originally developed to identify embryos at risk for genetic diseases. Today, however, they are primarily sold, at a cost of $6,000 to $12,000, as a way to screen for chromosomal abnormalities that could lead to failed implantation or miscarriages.
In October, however, a large study found that a single abnormal cell does not doom an embryo and determined that one of the tests, PGT-A, made no difference to rates of live births. Worse still, patients who opted not to transfer embryos based on the test’s results may have lost potentially viable ones.
There is also endometrial scratching, a procedure, sometimes costing as much as $500, that purposely irritates the endometrium, the innermost lining of the uterus, before IVF While it’s promoted as increasing the chance of an embryo implanting, a recent large randomized trial found no benefit. Beyond significant patient discomfort, risks include bleeding, infection and uterine perforation.
Then there are intralipids, an emulsion of soybean oil, egg phospholipids and glycerin administered intravenously and described as a way to decrease natural killer cell activation in the immune system and ostensibly aid in embryo implantation. This emulsion is priced around $400 per infusion; typically several are recommended. Side effects include headache, dizziness, flushing, nausea and the possibility of clotting or infection. A meta-analysis last year found that intralipids and other forms of immunotherapy should not be used in routine clinical practice.
Such procedures are often presented to patients in the form of a stack of papers, written in legalese or medical jargon. Resourceful patients might take to the internet to learn more, where searches might deliver densely written scientific articles, and ads might direct them to companies or clinics eager to promote their own brands of add-ons.
Why is all this happening? It’s because IVF remains an under-regulated arena, and entrepreneurial doctors and pharmaceutical and life science companies are eager to find new ways to cash in on a growing global market that is projected to be as large as $40 billion by 2024.
NYTimes.com, December 12, 2019 by Pamela Mahoney Tsigdinos
Click here to read the entire article.